NOMA AI · Health tech
HemoRisk
Designing an AI-powered clinical decision support system for maternal hemorrhage.
Overview
HemoRisk is an EHR-integrated clinical decision support tool designed to help labor and delivery teams assess maternal hemorrhage risk in real time. In this project, I designed a dashboard that translates complex AI predictions into clear, actionable signals, enabling clinicians to make faster and safer decisions in high-pressure environments. The work sits at the intersection of healthcare, machine learning, and safety-critical design, where clarity and trust are just as important as functionality.
The Challenge
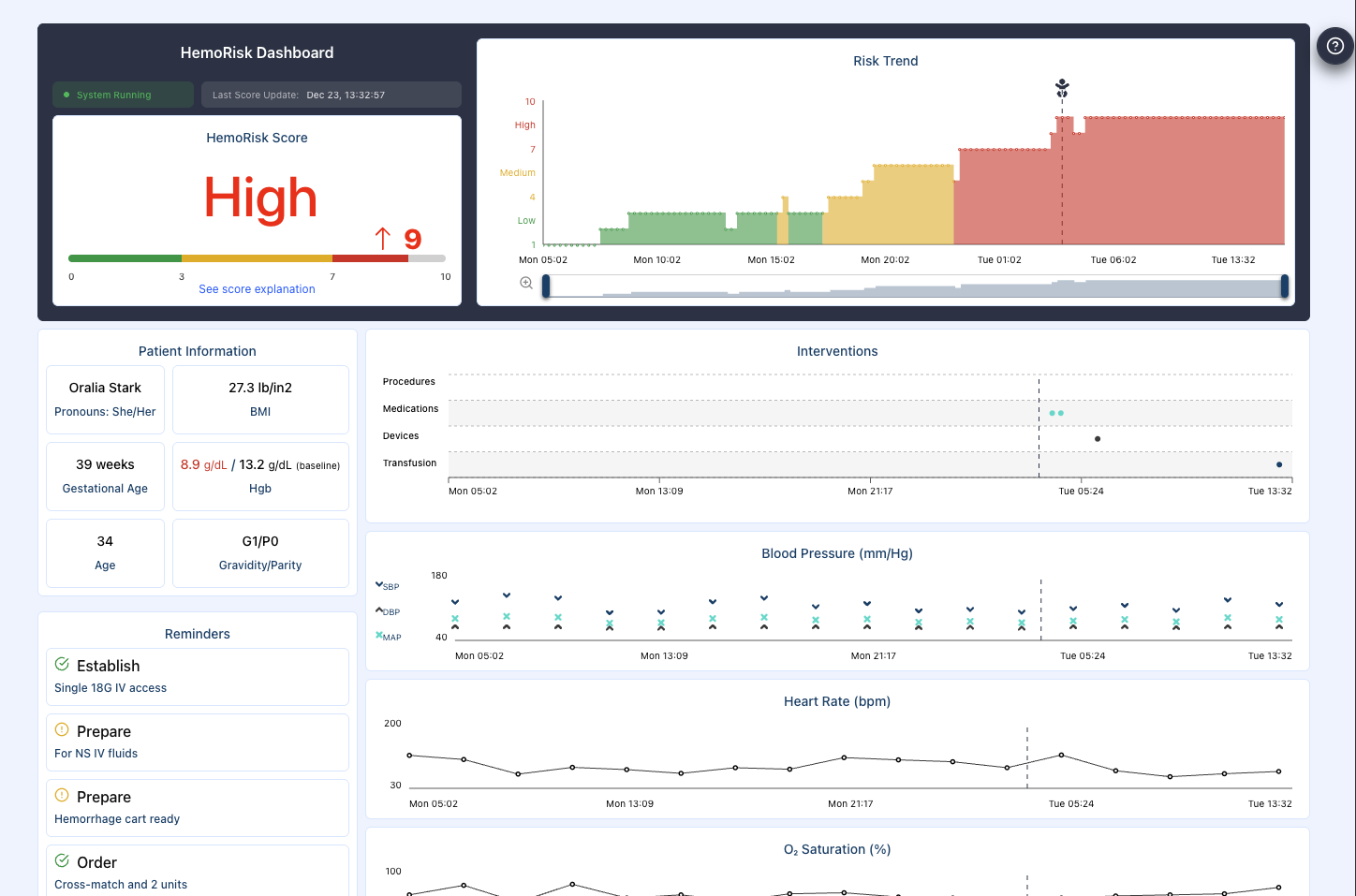
Maternal hemorrhage is one of the leading causes of maternal mortality, yet the tools clinicians rely on today are fragmented, manual, and difficult to interpret in real time. Risk assessments are often paper-based or mentally computed, and clinicians must piece together information across multiple systems while making time-sensitive decisions. This creates a gap between available data and actionable insight, where high-risk patients can be missed and changes in patient condition are difficult to track. The challenge was not simply to present more information, but to make the right information visible, interpretable, and trustworthy when it matters most.
The challenge was not just about presenting data. It was about designing for safety, trust, and clarity in moments where every second matters.
Understanding The Problem
Through early research, it became clear that clinicians were navigating multiple disconnected systems to gather patient information. Risk assessments were often paper-based or mentally computed, and detecting hemorrhage relied heavily on experience and estimation rather than standardized, real-time signals.
This created a dangerous gap between available data and actionable insight. High-risk patients could be missed, and even when risks were identified, there was often uncertainty about how those risks evolved over time.
My Goal
The goal of this project was to design a system that makes hemorrhage risk immediately understandable, fits seamlessly into existing clinical workflows, and builds trust in AI-driven predictions. At the same time, the design needed to support safe use in a high-stakes environment and meet FDA human factors requirements. This meant balancing usability, explainability, and safety without introducing additional complexity or disrupting how clinicians already work.


Research & Discovery
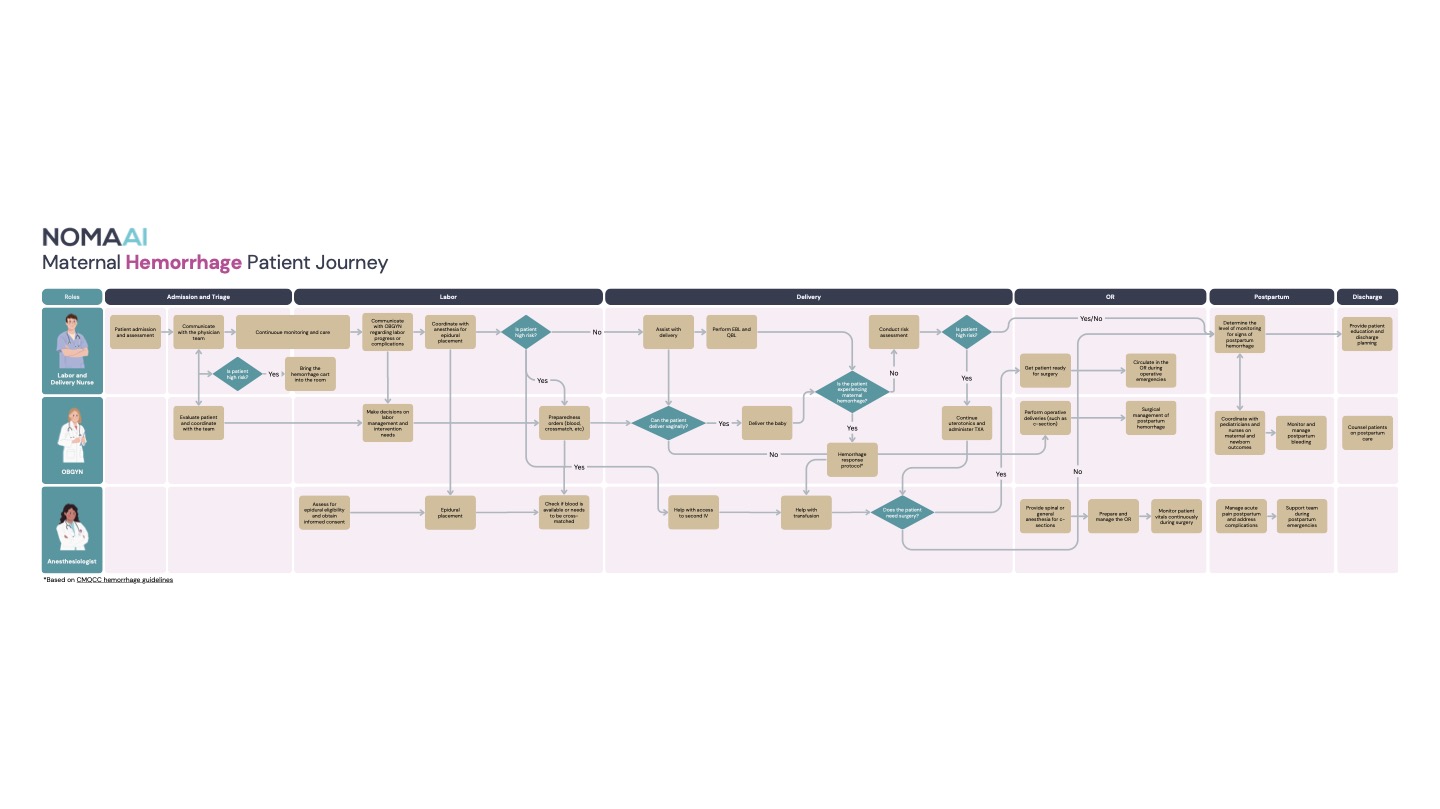
To understand how clinicians assess risk in practice, I conducted interviews with labor and delivery nurses, OB/GYNs, and anesthesiologists. Each role approached patient care differently, but all shared the same underlying need: quickly forming a clear understanding of a patient's condition without cognitive overload.
Mapping the clinical workflow revealed key breakdowns. Information was scattered across systems, communication between roles was not always synchronized, and recognizing changes in patient risk required constant mental tracking.
From this, a core insight emerged: clinicians did not need more data; they needed clearer actionable signals to make informed decisions.
Defining the Design Direction
Based on these insights, I focused on designing a single, integrated dashboard that could bring together patient data, AI-driven risk predictions, and clinical context in one place. The goal was to reduce switching between systems and make risk visible at a glance.
This direction was shaped by important constraints, including the need to integrate into existing EHR systems, preserve established workflows, and meet strict FDA requirements for usability and risk mitigation. These constraints were not limitations, but drivers that helped refine the design toward something practical and adoptable.

From Low to High Fidelity
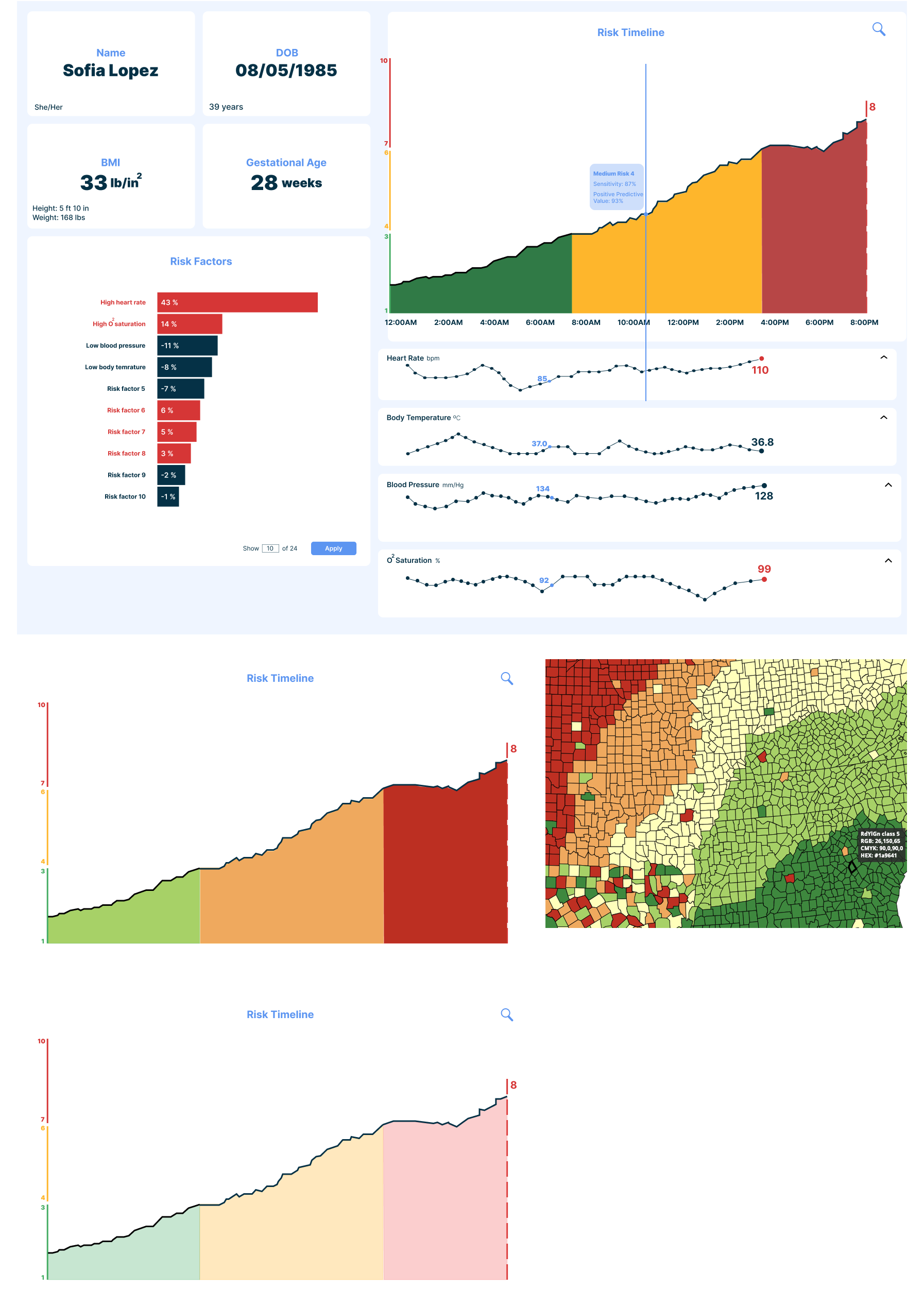
I explored multiple layout directions to understand how information should be structured and prioritized. Early prototypes focused on grouping related data, testing visual hierarchy, and evaluating how quickly clinicians could orient themselves.
As the design evolved, the hemorrhage risk score became the central anchor of the interface, supported by trend visualizations and contextual patient data. Every design decision was guided by a simple question: can a clinician understand this instantly under pressure?
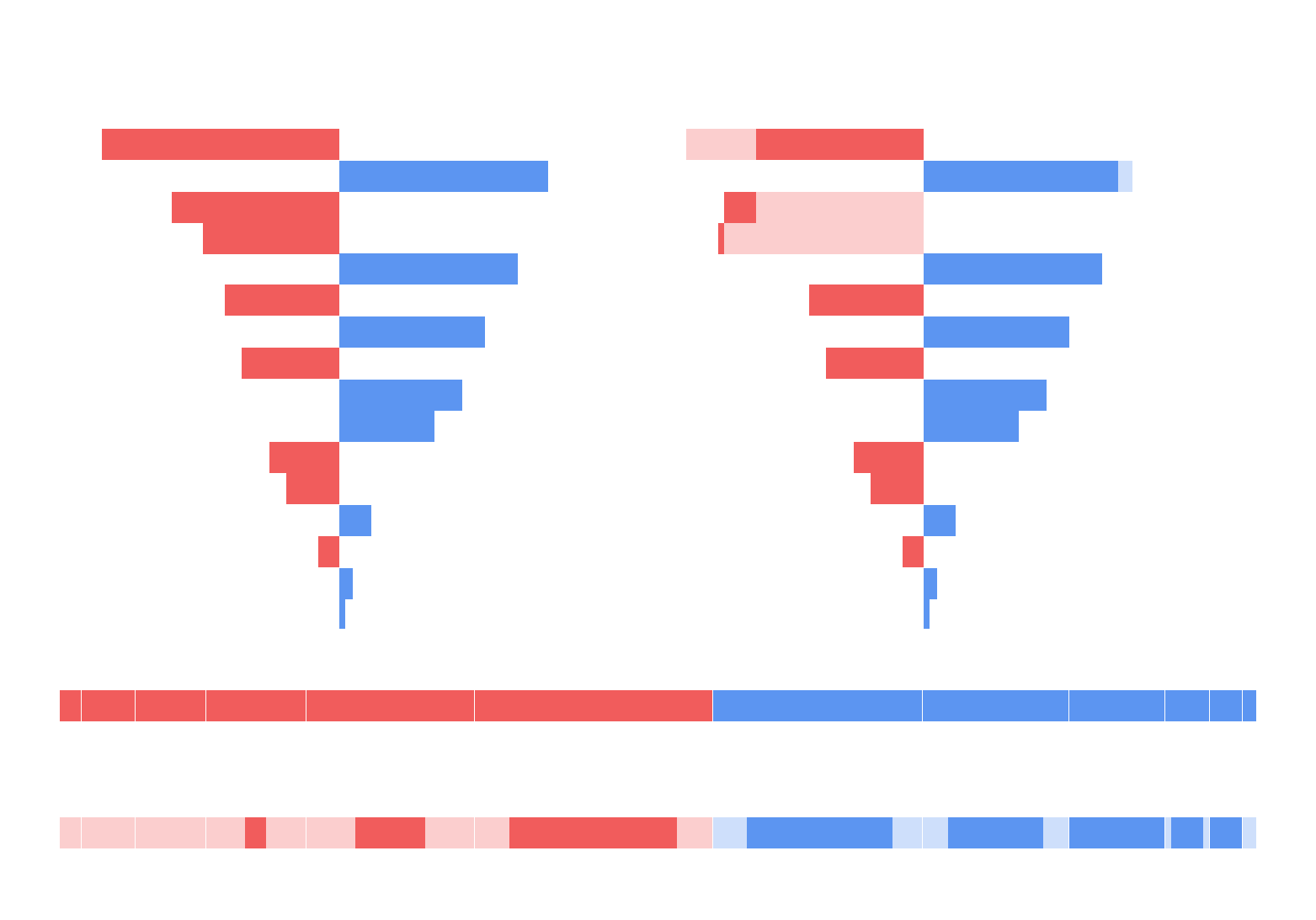
One of the most challenging aspects of the design was AI explainability. Clinicians needed to trust the system, which meant understanding not only the risk score but also the factors contributing to it. Through iteration, I translated complex model outputs into simplified visual explanations that could be interpreted quickly without requiring technical knowledge.
Final Design
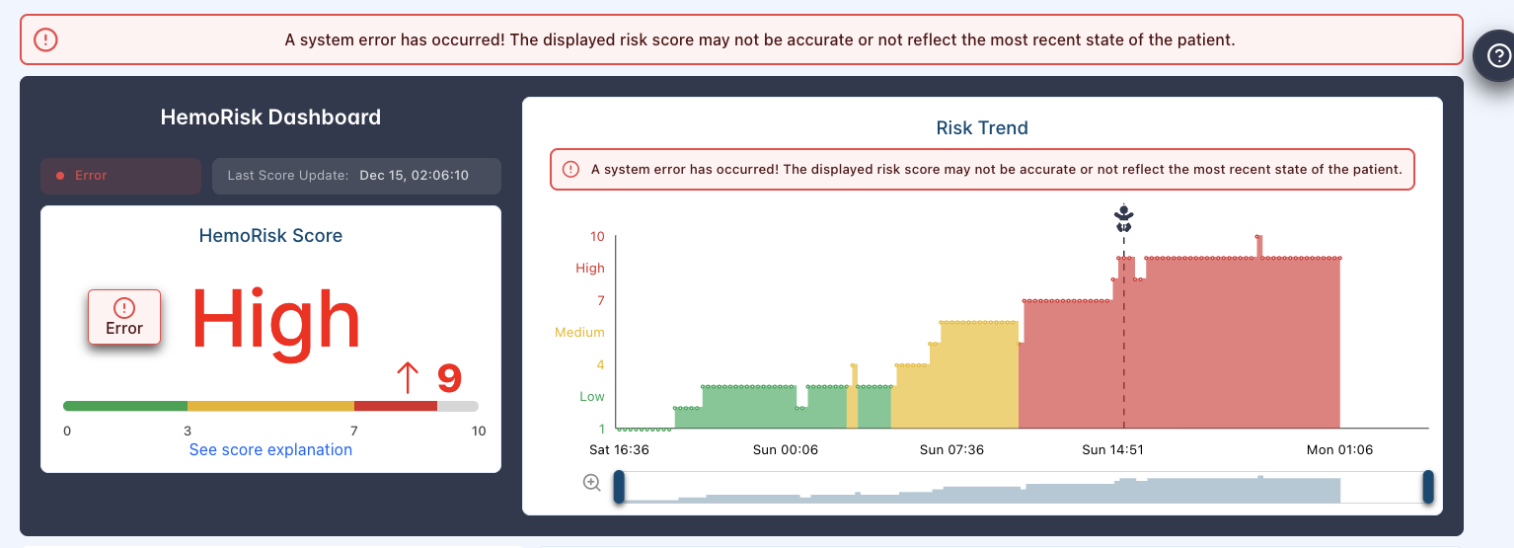
The final dashboard integrates the hemorrhage risk score, trend over time, patient vitals, and clinical context into a single, cohesive interface. Risk is persistently visible, and changes over time are easy to interpret through visual cues.
Supporting information is structured to provide context without overwhelming the user. The design prioritizes clarity, speed, and confidence, allowing clinicians to quickly understand what is happening and determine whether action is needed.

Designing for Safe Use
Unlike typical product design, this work required a strong focus on safety and risk. Because this is a safety-critical product, I conducted a User-Related Risk Analysis to identify potential use errors and evaluate how interface decisions could impact clinical outcomes.
Every interaction, label, and visual element was assessed in terms of its potential to introduce misunderstanding or delay decision-making. This process ensured that the design not only works well, but actively supports safe and correct use.
Validation
To validate the design, we conducted a summative usability study aligned with FDA human factors guidance. Clinicians were asked to complete realistic tasks without prior training, simulating real-world adoption.
The results showed that most participants were able to successfully complete tasks on their first attempt and described the system as intuitive and easy to use. When failures occurred, they were typically related to small interface details rather than misunderstandings of clinical risk. This indicated that the design supported safe and effective use, even for first-time users, while also highlighting opportunities for refinement.

Impact
HemoRisk enables earlier detection of maternal hemorrhage risk by combining real-time clinical data with AI-driven insights in a single, integrated interface. By reducing cognitive load and eliminating the need to navigate multiple systems, the design supports faster and more confident decision-making.
More broadly, the project demonstrates how thoughtful design can bridge the gap between complex machine learning systems and real-world clinical practice, making advanced technology usable in high-stakes environments.